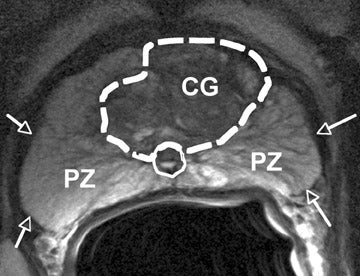
Top: Image of MRI scan using 3T machine identifying possible carcinoma sites. Below right: MRI machine similar to the one I was in yesterday.
Yesterday afternoon I experienced my first MRI scan done as a prostate exam recommended by my oncologist in San Francisco. This was after the post treatment PSA recently spiked to 6.0. See e.g.
http://brane-space.blogspot.com/2016/05/post-treatment-psa-spikes-to-60-not-so.html
In the wake of seeing these results the UCSF oncologist ordered an MRI exam, as opposed to a prostate biopsy and with good reason: given the tissues of the prostate have already been exposed to high dose (Ir 192) radiation, (1920 cGy) they will be scarred and much more susceptible to hemorrhage.
In addition, MRI technology has proceeded so markedly in the last ten years (due to what is called faster development of "echoplanar surfaces" - or MRI image slices) that the MRI can now actually find and grade carcinomas that occur there. The key has been the development of more powerful 1.5- and 3-Tesla scanners where Tesla refers to the magnetic field strength. (1 T = 10,000 Gauss). The machine that scanned my pelvic region was 3T or fifteen times greater than the magnetic field of the most powerful sunspots.
The result has been a quantum leap in signal to noise ratio (or "SNR") with the SNR increasing with magnetic field strength. Thus, the 3T (and 1.5T) machines are ideally suited to the task of scanning for prostate lesions.
According to one radiology website:
"Current receiver coil technology includes pelvic phased-array coils with or without the addition of an endorectal coil. The endorectal coil adds approximately an order of magnitude to the available SNR and also allows for the use of small fields-of-view (FOV) for some critical applications"
The endorectal coil is actually a thin wire inserted inside a balloon filled with 50 ml of air to fix the coil to the prostate for better reception of the radio frequency waves and superior SNR. However, much of the literature so far disputes these ERCs improve imaging that much over what an external pelvic coil delivers.
In my case, at Penrad, only the outer pelvic array coil was used not the ERC, and I was glad for that - given the use of the latter too necessitates having an enema first, then having the ERC inserted inside a condom. Thus, according to the same radiology site noted above:
"the endorectal coil is highly preferred, even though it adds discomfort, time, and cost to the MR exam"
Anyway, after arriving I was greeted by a young blonde woman who allowed Janice to accompany me and took my paperwork which included ensuring I had absolutely no metal artifacts anywhere in me (like implants or pacemakers) or on me. Next, I had to assure her I was not claustrophobic - because many people freak out when being put into an MRI for the first time, given the tightly confined space (6" from your face). Also, you can't move at all during the process when can take from 20 minutes to an hour. So you're basically "trapped" in that space for up to an hour - but you are handed a little "squeeze" alarm in case you do panic.
After taking all my insurance and other data down the young woman escorted me to a changing room and told me I had to remove all my clothing and put them in the locker provided - which she pointed to. She then opened another door and showed me the two sizes of surgical gown. Already, with all this huff and puff, I was starting to get nervous that I might have to be "introduced" to the ERC! Fortunately that was not the case, and as the woman left Janice helped me into the stupid gown - which was the only thing covering me.
After finishing I peered outside to see three young women all seated in their own gowns but allotted more clothing (like shoes, etc.) than I was. I balked at first going out, but Janice accompanied me staying close so none of the women could see too much. So in that condition I had to sit and wait with these women until called. Janice kept my mind off my embarrassing state by using her Ipad to bring up different restaurants to go to afterwards.
After twenty minutes or so my name was called, whereupon I was walked to the MRI room and assisted onto the table. My head fitted snugly into a cushioned support and my legs were raised on the MRI table, as the pelvic array coil was spread on top. I was then given earphones and chose some piped in music (60s rock) to drown out the loud 'banging' sound of the MRI. (It was somewhat like being in a giant tin can with huge hammers banging different tones while you lay still).
The scanning began and I enjoyed the music but found it difficult to catch a breath. Finally, after about 16 minutes I tried to slowly inhale and exhale when the operators stopped and warned about taking deep breaths. So she had to run those slices over again. Then about ten minutes later the scan suddenly stopped once more and I was asked to please use the rest room just outside as the MRI scans were picking up gas (trapped in the rectum) obscuring the images. I complied and returned after expelling roughly two loud farts.
Assisted back onto the MRI table, the scanning resumed where it left off and was completed in about ten minutes with no further issues. I was told the imagery - on a CD- would be sent to my primary doc and would be available in about 1-2 days. I then ambled back to the waiting room - where Janice was- to change back into my clothes. From there it was on to the Texas Roadhouse restaurant where we enjoyed two excellent steak dinners.
What happens next will depend on what the MRI scans show. I told Janice that at the least they will likely show the same 6 cancerous cores - at grade T1C - that were first detected in my standard biopsy 4 years ago. (The MRI, of course, is unable to render the Gleason score).
Basically, if the imagery shows the disease is "indolent" I plan to adopt a wait and see approach, probably continuing with the PSA tests and getting the occasional MRI. But NO more biopsies for the reason already given.
If the cancer (adenocarcinoma) is found to have spread I will then wait until evidence of metastasis - before considering androgen deprivation therapy (ADT) since new research finds little difference in benefit between initiating it right away and once bone metastasis has arrived. The advantage of ADT - even if used in cycles (which I will likely do because of the nasty side effects, e.g. depression, loss of memory, metabolic disease, cardiac problems, high BP etc.) is to lessen risk of bone fractures. Once the cancer spreads to the bones further metastasis naturally will weaken them and increase fracture risk.
But as I said, I am opting here for life quality as opposed to quantity. My will has already been revised and the estate lawyer is working on the final draft including a revised living will and advanced directive "to take into account what occurred in the Terry Schaivo case". The primary change in the will was to the beneficiaries and also a more exhaustive accounting of assets.
I may have two years left or ten, I don't know and can't say. But the only choice any of us has is to keep on keeping on and try our best to live each day to the fullest - as we define that term.
To see a video explanation of the MRI process. including the sort of sounds you hear:
https://www.youtube.com/watch?v=DZTXa4qerI4
No comments:
Post a Comment